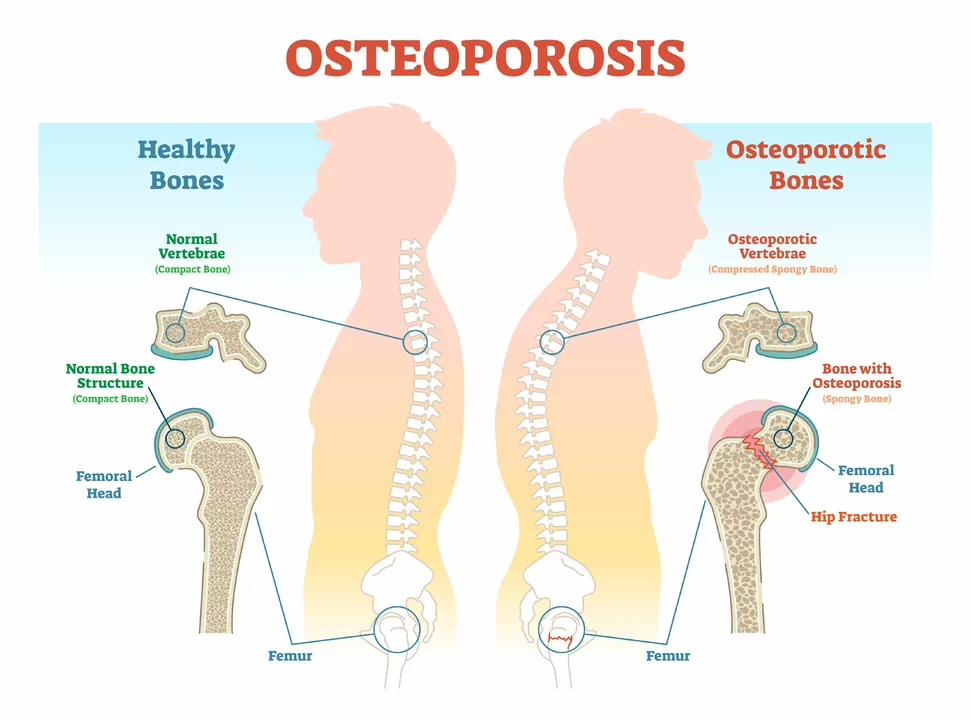
Bone Health: Practical Tips to Strengthen Your Bones
Bones aren’t lifeless scaffolding. They change, repair, and yes—get weaker if you don’t treat them well. Want to lower your fracture risk and keep moving? This page gives simple, useful steps you can use today: what to eat, how to move, when to check with a doctor, and common meds and supplements to know about.
Quick wins: diet and supplements
Calcium and vitamin D matter. Aim for about 1,000–1,200 mg of calcium daily from food first—milk, yogurt, canned salmon with bones, and leafy greens. If you don’t get enough from food, a supplement can help. For vitamin D, many adults take 800–2,000 IU daily depending on levels and sun exposure. Ask your doctor for a blood test before starting high doses.
Protein and vitamin K also support bone repair. Eat lean protein, beans, and plenty of vegetables. Avoid crash diets that cut out key nutrients—your bones need steady fuel.
Move the right way
Weight-bearing exercise helps bones get stronger. Try brisk walking, stair climbing, dancing, or light jogging. Add strength training 2–3 times a week—simple moves with bands or dumbbells build muscle and protect joints. Balance work matters too: yoga, tai chi, or single-leg stands cut the chance of falls.
Start slow if you’re new to exercise. Even short daily sessions add up. If you have pain or a diagnosed condition, check with your doctor or physical therapist for a safe plan.
Know the meds that affect bones. Long-term steroid use can weaken bones. Some anticonvulsants, certain cancer treatments, and proton pump inhibitors may also change bone density. If you take these drugs, talk to your doctor about monitoring and prevention.
Screening and treatment: when to act. If you’re a woman over 65 or a man over 70—or younger with risk factors—ask about a bone density (DXA) scan. If tests show low bone density, treatments like bisphosphonates, denosumab, or other options can cut fracture risk. Every treatment has pros and cons; ask about side effects and how long you should be on a medicine.
Small changes at home prevent big problems. Improve lighting, remove tripping hazards, put grab bars in the bathroom, and wear sturdy shoes. Check your vision and review meds with your doctor—some can cause dizziness and increase fall risk.
Want practical next steps? Start with a food diary for a week, add two 20-minute walks, and book a check-up if you’re on steroids or have had a fall. Bone health improves slowly, but steady habits matter.
Explore our articles on supplements, medication guides, and rehab tips to learn more about specific treatments and everyday fixes for stronger bones.