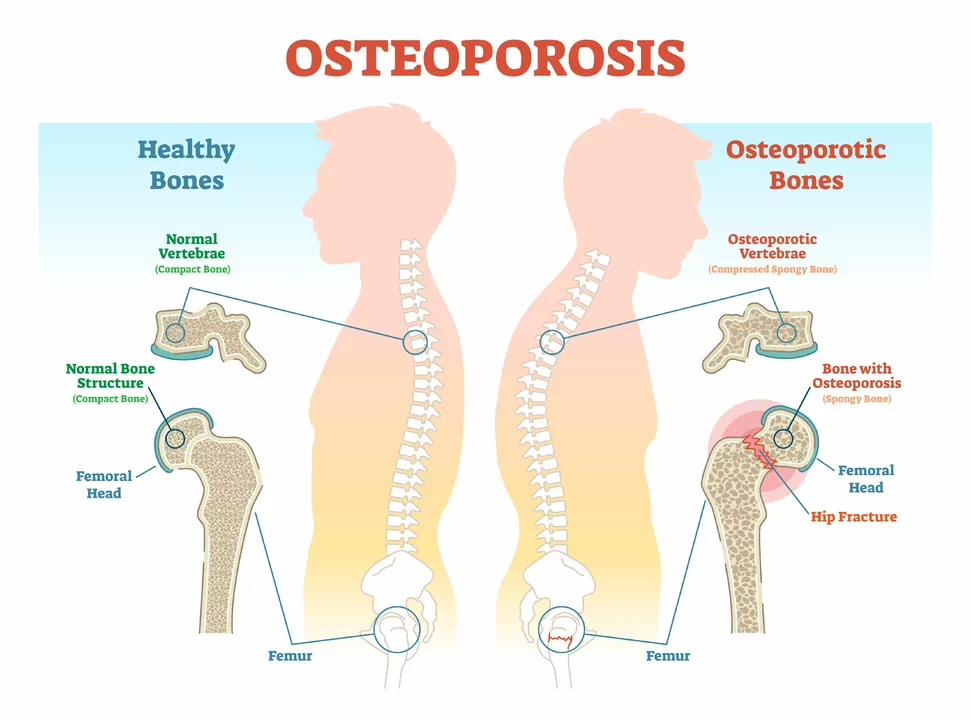
Osteoporosis — what to watch for and what you can do
About 1 in 3 women and 1 in 5 men over 50 will break a bone partly because of weak bones. Osteoporosis makes bones fragile without obvious pain until a fracture happens. That’s why spotting risk factors early and taking simple steps can make a big difference.
How osteoporosis is diagnosed
Your doctor will usually start with a risk check: age, menopause, family history, long-term steroid use, smoking, heavy drinking, low body weight or previous fractures. If risk is present, the standard test is a DXA (dual-energy X-ray absorptiometry) scan. It measures bone density and gives a T-score. A T-score of -2.5 or lower means osteoporosis; between -1.0 and -2.5 is called osteopenia (low bone mass).
Blood tests may follow to rule out secondary causes: low calcium or vitamin D, thyroid issues, or conditions like celiac disease. If you’re on steroids or have lost height, mention it — that speeds up evaluation.
Treatments and everyday steps that help
Medications can cut fracture risk and are usually considered if your T-score shows osteoporosis or if you’ve already had a fragility fracture. Common options include:
- Bisphosphonates (alendronate, risedronate) — often first choice. They slow bone loss.
- Denosumab — an injection every 6 months. Works fast but needs careful stopping plan to avoid rebound bone loss.
- Bone-building drugs (teriparatide, romosozumab) — used when the fracture risk is high or other drugs didn’t work.
- Raloxifene or hormone therapy — may suit some postmenopausal women but carry other risks to discuss with your doctor.
All meds have pros and cons. Rare side effects (jaw issues, unusual thigh fractures) are possible. Talk through options and monitoring with your clinician.
Alongside drugs, these practical moves help right away:
- Get enough calcium (total 1,000–1,200 mg/day from food and supplements) and vitamin D (often 800–2,000 IU/day — check levels with your doctor).
- Do weight-bearing and resistance exercises 3–4 times a week (walking, stair climbing, light weights). Add balance and flexibility work to reduce falls.
- Stop smoking and limit alcohol — both speed bone loss.
- Fall-proof your home: clear trip hazards, add grab bars, improve lighting and wear sensible shoes.
- Keep protein intake adequate to support muscle and bone repair.
If you’re on long-term steroids, have early menopause, a parent with hip fracture, or unexplained height loss, ask for a bone check sooner than age 65. After any low-impact fracture, get evaluated — treatment can prevent the next one.
If this sounds like your situation, make an appointment and ask about a DXA scan and bone-friendly steps you can start today. Small changes now can prevent big problems later.