Raynaud's Phenomenon: What It Looks Like and How to Manage It
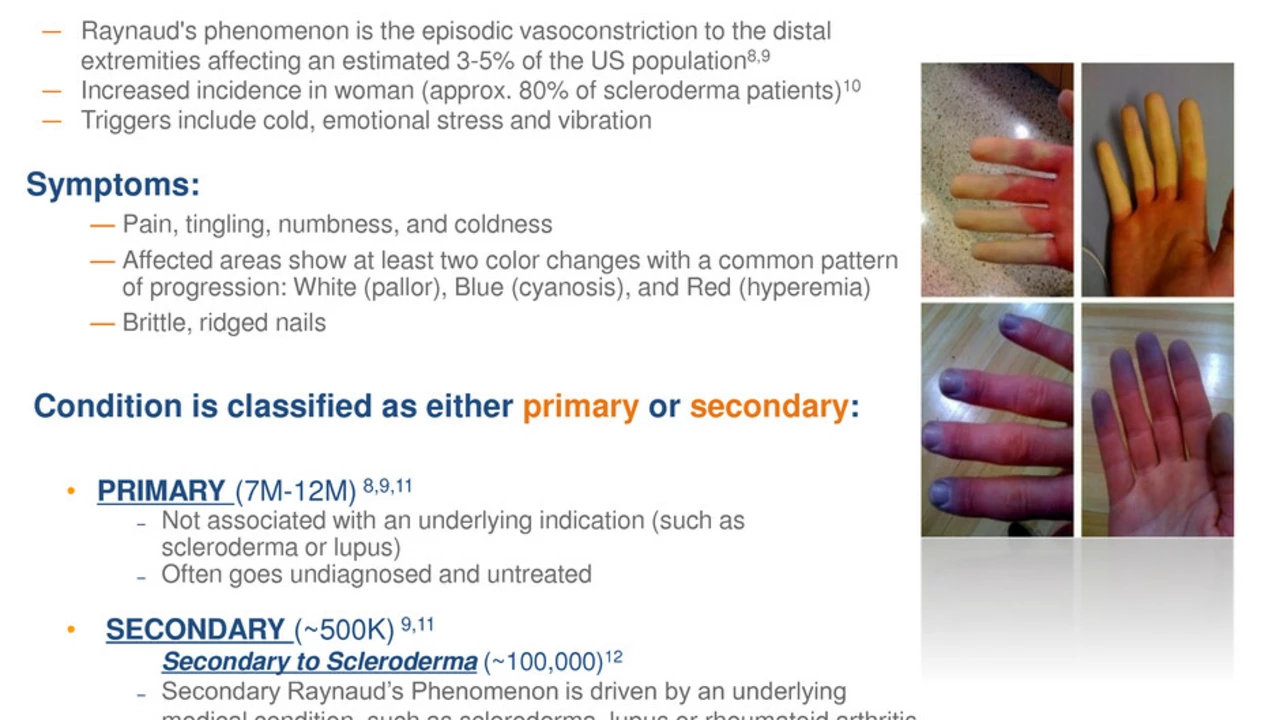
Raynaud's causes sudden color changes in fingers and toes when you get cold or stressed. They often turn white, then blue, then red as blood flow stops and returns. It feels numb, tingly, or painful during attacks. Knowing what triggers attacks and how to act fast can cut discomfort and prevent skin damage.
Primary vs Secondary — why it matters
Primary Raynaud's is the common, milder form and usually isn't linked to other diseases. Secondary Raynaud's happens with conditions like scleroderma, lupus, or rheumatoid arthritis and can be more serious — ulcers or tissue damage are possible. If your symptoms start in adulthood, get worse over time, or include skin sores, ask your doctor about testing.
Quick, practical steps that help
Warm first, then protect. When an attack starts, move to a warm place if you can. Put your hands in warm (not hot) water, rub them together, or cup them over a warm drink. Dress in layers: wear insulated gloves and a warm hat — heat escapes through the head and makes extremities colder. Chemical hand warmers or battery-heated gloves are handy for long outdoor exposure.
Cut the common triggers. Stop smoking and avoid secondhand smoke — nicotine tightens blood vessels. Watch stimulants: high caffeine or certain cold medicines with decongestants can worsen attacks. Try to reduce stress with simple breathing or short walks; emotional stress can trigger vasospasm.
Protect your hands at work and home. Use mittens instead of thin gloves for truly cold days. When handling cold objects (like frozen food), wear insulated gloves. If you wash dishes in cold water, wear rubber gloves with a warm liner inside.
Medical options to discuss with your doctor. First-line drugs are calcium channel blockers (nifedipine or amlodipine) — they relax small blood vessels and reduce attack severity. Topical nitrates can help some people for local relief. In severe cases or with ulcers, doctors may suggest vasodilators like sildenafil, IV prostaglandins, or rarely, surgical sympathectomy. Always ask about side effects and interactions.
When to see a doctor. Make an appointment if attacks start suddenly as an adult, get more frequent, cause sores, or if you have symptoms of an autoimmune disease (new joint pain, rashes, dry eyes). Your doctor may order blood tests (ANA, ESR, rheumatoid factor) or a nailfold capillaroscopy to look at tiny blood vessels.
Living with Raynaud's means planning ahead. Pack warm accessories when you travel, keep a hot-pack in your car, and tell your workplace about simple adjustments you need. Small habits — warm drinks, avoiding tight rings, steady exercise to improve circulation — add up.
If you want, bring a short symptom diary to your next visit: note what triggered each attack, how long it lasted, and what helped. That makes it easier for your clinician to tailor treatment and decide if more tests are needed.